For nearly a month, nine-year-old Mariatu Koroma had not been herself.
She was usually playful and talkative, her mother, Adama Kamara, says. But gradually she became quiet, stopped playing, and grew thinner.
“She was not the same child,” Adama says.
At first, the changes were subtle, but over weeks, the weight loss became obvious. Her clothes hung loosely, she tired easily, and she could no longer keep up with other children.
They first sought care at a hospital close to home, where Mariatu was admitted for two weeks. There were suspicions of intestinal worms and later concerns about a heart condition, but she did not improve.
Each passing day without answers increased Adama’s worry. She watched her daughter weaken and did not know why.
A neighbor advised Adama to try PIH-supported Koidu Government Hospital in Kono District.
When Mariatu arrived on January 27, she was weak and visibly ill. Immediate tests in the Pediatric Emergency unit showed her blood sugar was dangerously high. Further testing revealed that her body had begun producing harmful acids because it could not properly use sugar for energy.
She was diagnosed with diabetic ketoacidosis, a life-threatening complication of diabetes.
Community Health Officer Hawa Kamara remembers how critical she was on arrival.
“If it is not treated quickly, it can be fatal,” Hawa says.
Mariatu was immediately started on insulin and closely monitored. Her fluids were carefully managed to stabilize her condition. For several days, she was not allowed to eat while her body regulated. . Malaria and a urinary tract infection were also treated, as these likely worsened her condition and triggered the crisis.
The first days required constant monitoring. Blood sugar levels were checked frequently, and her breathing, pulse, and level of alertness were closely observed.
After six days, the dangerous acids cleared from her body. Her condition stabilized, she could now be transitioned to insulin injections under the skin.
For Adama, the diagnosis was frightening.
“I was afraid when they told me it was sugar,” Adama says. “I know it is a serious and complex condition.”

The PIH-supported Koidu Government Hospital officially launched its expanded Non-Communicable Disease (NCD) clinic on 4th of February 2025 to meet the demand of the growing number of patients.
Photo by Chiara Herold / PIH
Dr. Bernard Samuel Kakala, clinical mentor in the Non-Communicable Diseases (NCD) clinic at KGH, explains that Mariatu has Type 1 diabetes, a condition in which her body does not produce enough insulin. That means she will be reliant on insulin for the rest of her life.
The NCD clinic is a dedicated space for long-term management of conditions like diabetes and hypertension. For many families in rural districts like Kono, managing a chronic illness can be overwhelming. Regular medication, monitoring equipment, and transport to clinic visits can place a heavy burden on households already facing economic challenges.
Before its establishment, patients with chronic illnesses were often seen in general outpatient settings without structured follow-up. Today, one year after opening the doors of its expanded facilities, the clinic provides scheduled appointments, medication refills, ongoing monitoring, and education under one coordinated system.
As of December 2025, the clinic had enrolled 153 children living with Type 1 diabetes, each requiring daily insulin injections and regular monitoring for the rest of their lives.
When treatment means lifelong changes, education is a crucial first step before discharge from the hospital.
“Sometimes a child is the first one in the family to have diabetes,” Dr. Kakala explains. “There are many myths in the community, so we have to teach them clearly what this disease is and why it happens.”
Mariatu and her family were trained by staff on how to inject insulin, how to monitor her blood sugar, and how to recognize warning signs of both low and high sugar levels. The clinic provided her with insulin, a glucometer, test strips, and a logbook to record her readings.
“When she comes back, we will review the logbook to understand the trend,” Dr. Kakala says. “From there, we adjust the insulin if needed.”
Insulin must be stored carefully. Ideally, it should be kept between two and eight degrees Celsius, or 36 to 46 degrees Fahrenheit. But many families do not have refrigerators.
“For most people, we try to find a local way,” he says. “Insulin can usually be stored in cold water, or an ice bar can be used to keep it cool. Alternatively, it can be placed in a geometry box [a small, insulated cooler box] and kept on the ground in a shaded area away from sunlight.”
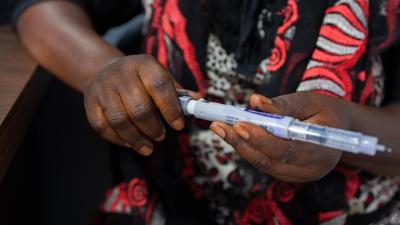
Dumaneh Kabba, a patient living with Type 1 diabetes since 2020, receives care at the Non-Communicable Disease (NCD) Clinic at KGH. During her appointments, nurses support her in administering insulin.
Ibrahim John Kamara / PIH
The clinic supplies medication for about one month at a time. At each follow-up visit, the team reassesses blood sugar control and reviews any challenges the family may be facing.
Patients are also connected with peer groups of people living with diabetes.
“When they share their challenges, they realize they are not alone,” Dr. Kakala says.
Because diabetes requires lifelong treatment, the team also works to address the practical barriers families may face in maintaining care. For families who struggle with transport or food, social workers can assess and provide support when needed. In Mariatu’s case, her family is currently able to manage follow-up visits independently.
Today, Mariatu checks her own blood sugar. She understands what the numbers mean and knows how to inject insulin with supervision.
She is still adjusting to a new routine, but she is no longer the child who arrived visibly ill.
Her life may now include monitoring, follow-up visits, and a logbook filled with numbers, but it will also return to fun things like school, family, and play.
Adama keeps the hospital’s phone numbers carefully written down, just in case she needs someone urgently. She is also ready to go and spread the word about KGH in her village.
“If my neighbor had not told me to come here, I wouldn’t have known to,” she says, adding, “and that’s why I have to ensure I do the same for my other neighbors too.”
For Hawa, children like Mariatu represent both challenge and hope.
“We are hoping for an expanded pediatric complex with a dedicated ICU,” she says. “This room is currently serving as both an ICU and a resuscitation center. Sometimes we are overwhelmed by how insufficient the space is.”
Still, every week, children like Mariatu leave stronger than they arrived, and mothers like Adama return home with relief.



